 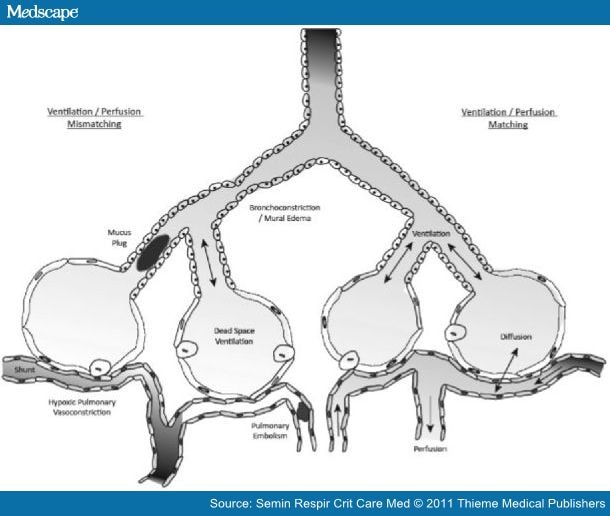
In physiologic dead space, alveoli are ventilated but not perfused. Physiologic Dead SpaceĪ second type of dead space, physiologic dead space, consists of alveoli that are ventilated but lack capillary blood flow to pick up oxygen and drop off carbon dioxide. For another clinical explanation of how hypoventilation causes hypoxia and the difference between oxygenation and ventilation click here. It’s important to realize that by providing extra oxygen, a good practice, you delay the onset of hypoxia, but you may also delay the diagnosis of dangerous hypoventilation if you’re not looking for it. Respiratory rate eventually slows and the patient can stop breathing. This worsens hypoventilation, and increases carbon dioxide even more. So all other things being equal, a PCO2 of 70 is associated with a pH of 7.1. If carbon dioxide rises into the 70–80mmHg range it will also profoundly sedate the patient. Each 10 mmHg change in PCO2 roughly changes your pH by 0.1. Hypoventilation leads to increased PaCO2.Īcute values above 50 mmHg are significant and require treatment, values above 70 mmHg can be life-threatening because of respiratory acidosis among other things. As a result, her carbon dioxide starts to rise. However, she is barely moving her dead space gas back and forth so her ventilation is poor. If you’re providing our baby with extra oxygen, she may not become hypoxic right away because enough oxygen will still reach her alveoli to maintain her oxygen saturation for a while. If you breathe a high concentration of oxygen, but don’t increase or decrease your respiratory rate, your arterial oxygen content (PaO2) will greatly increase, but your PaCO2 won’t change. Oxygenation is simply the addition of oxygen to the body. Ventilation exchanges air between the lungs and the atmosphere so that oxygen can be absorbed and carbon dioxide can be eliminated. Remember, oxygenation and ventilation are different. Her dead space is still 8 so now the amount of gas reaching her alveoli is 2 ml (10 ml – 8 ml). She’s still moving 10 ml of gas in and out of her mouth and you can feel her breathing and see her chest move, even though it looks shallow. She starts to hypoventilate and is now breathing tidal volumes of 10 ml. Let’s say our baby is sick with nausea, vomiting, and a fever of 101F (38C). So again that’s 14 ml of air reaching the alveoli and 8 ml being effectively wasted. For our baby, the anatomic dead space is 8 (3 X 2.7). Our teenager will have an anatomic dead space of 120ml (2 ml/kg X 60 kg), which means that of his 480 ml breath, roughly 360 reaches the alveoli and 120 doesn’t participate in exchange gas at all. Let’s look at an example of how anatomic deadspace impacts adequacy of breathing.Īnatomic dead space is an important concept in determining if tidal volume is adequate. about a tablespoon - an impressive difference. In terms of liquid volume, that’s a can of soda vs. A healthy infant weighs about 2.7 kg (6 lb) will have about 22 ml alveolar ventilation. An adequate tidal volume must include enough volume to also fill the deadspace, otherwise not enough air enters the alveoli and the patient hypoventilates.Ī healthy teenage boy weighing 60 kg (132 lb) will have about 360 ml of alveolar ventilation. It’s highest in the infant at 3 ml/kg ideal body weight and is about 2 ml/kg in older children and adults. It’s called anatomic because it’s fixed by anatomy and doesn’t change.Ībout a third of each normal breath we take is anatomic dead space, which means that a third of each breath is essentially wasted. It consists of conducting airways such as the trachea, bronchi, and bronchioles -structures that don’t have alveoli. Anatomic Dead SpaceĪnatomic deadspace consists of the parts of the respiratory tract that are ventilated but not perfused. They all impact how well a patient ventilates. There are three types of dead space: anatomic, physiologic, and that dead space belonging to any airway equipment being used to assist ventilation. Dead space is the portion of the respiratory system where tidal volume doesn’t participate in gas exchange: it is ventilated but not perfused. One important contributor to ventilation perfusion mismatch is dead space. It will help you understand how you can use these concepts to care for your patient. This article will describe how dead space is different from shunt. Physiologic dead space is ventilation of poor perfused alveoli. Shunt is perfusion of poorly ventilated alveoli.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
